Playlist
Show Playlist
Hide Playlist
Cellular Response: Introduction
-
Slides Acute and Chronic Inflammation Cellular response.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
00:01
Welcome.
00:01
The topic for discussion
is all about
the cellular response
in acute inflammation.
00:07
We've previously talked about
the vascular response.
00:10
And now we're going to bring in
the neutrophils.
00:13
The acute inflammatory cells that
are going to clean up the mess
that happened when we had injury
and start the healing response.
00:24
The cellular response involves
neutrophil recruitment,
so getting them in
to the area of injury.
00:30
Once they're there,
they have to phagocytized,
they have to eat,
and they have to kill.
00:36
And they will also have mediators
that they will release
that will be important
in this inflammatory response.
00:43
Those mediators include
reactive oxygen species,
that we've talked about before,
ROS.
00:47
ROS are very important
in this process.
00:50
And we'll cover that in detail.
00:52
They also elaborate proteases
to degrade the debris
that has been part of the injury
in that location.
01:00
And they will elaborate
a number of other mediators,
including importantly
eicosanoids.
01:05
And we'll spend
a fair amount of time
talking about eicosanoids.
01:09
There are lots of details here.
01:11
There are lots of
very important things
that we will be interested in.
01:16
So hang in there, keep in mind,
these basic kind of buckets
of what we're going to talk about.
01:23
The first thing is getting
the neutrophils in to the tissue
of the area of injury.
01:28
So this is our vascular bed.
01:29
We have coming from
the left side into the right side,
we have arteriole
that branches into capillaries,
that then comes into back together
into the postcapillary venule.
01:40
There are a few cells
that are normally
in the extravascular matrix,
lymphocytes,
and macrophages.
01:48
There will also be mast cells
and other tissue types of cells.
01:53
When we have
acute inflammatory responses
in response to injury,
what we've already discussed
is that increased vascular flow.
02:03
so we have dilation of the arteriole
and increase flow into the tissue.
02:08
This provides greater blood
into the area of injury.
02:12
The entire bed of vessels
gets more dilated.
02:16
So that will be apparent grossly as
calor (heat), and rubor (redness).
02:23
And there will also be increased
vascular permeability,
as we've talked about,
as we increase
the hydrostatic pressure.
02:29
We've also now in this
vascularized area
of cellular inflammation,
we've recruited and have neutrophils
that have left the blood vessels
and are in the tissue.
02:40
And they are looking around,
for where's the damage,
and how can they help
clean it up?
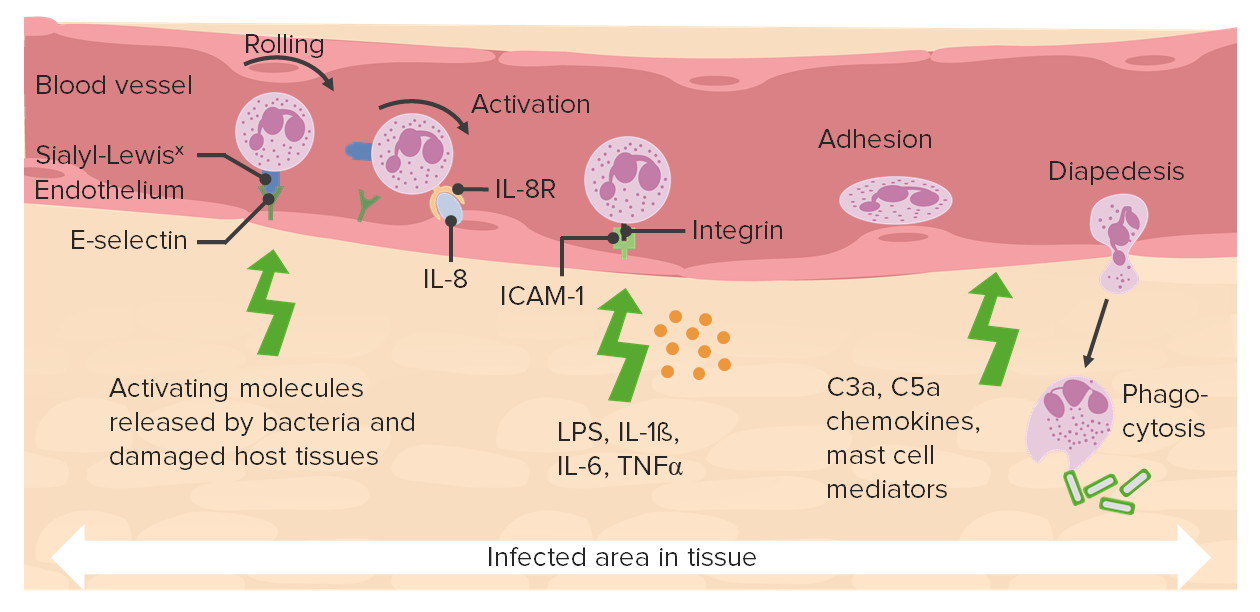
So the next process
that we're going to talk about is,
how do we get the neutrophils there?
This is going to be a complex kind
of animation
that we will walk through
to look at
how neutrophils,
and other inflammatory cells
can lead the bloodstream,
and get into the area
where there has been injury.
03:08
So what we're looking at essentially
is the endothelium,
that's that yellow line
near the bottom,
it sits on a basement membrane
and below
it is the extravascular matrix.
03:17
And above that in the bloodstream,
would be a leukocyte.
03:20
And we're going to have blood flow
going from right to left.
03:24
So, what we have here
is a leukocyte
not at surface
or a variety of molecules,
those will become important
in a minute.
03:31
Okay.
03:32
We need to somehow
tell the leukocyte,
"Come here.
Dive into this spot."
And that involves cells
that are acting as sentinels
that live in the
extravascular space,
mast cells, and macrophages,
will respond to injury.
03:48
And we'll talk about
how that happens.
03:50
But we'll respond to injury
and make a variety of mediators
that will turn on the endothelium
and make it sticky.
03:57
And that will be a cue
to the leukocytes
that this is where
they need to go.
04:02
Macrophages and mast cells
are also going to make
the vessels leakier.
04:06
So the endothelium
will pull slightly apart
and we will get fluid
that comes out.
04:10
As a result of that,
we get stasis.
04:13
We get a relative
sluggishness of the blood
because a lot of the
extra water and electrolyte
has flowed out into the tissue.
04:20
That's the tumor that we talked
about previously, the edema,
that's associated with
the vascular response.
04:26
By making the blood flow sluggish,
now those leukocytes
that are zipping by
start bouncing along the surface
of the endothelium.
04:36
That's the next step,
that's rolling.
04:38
And we'll talk about how the various
molecules on the endothelium
and on the leukocyte are involved
in that rolling process.
04:46
The leukocyte will roll for a while
and then driven by
additional molecules
chemokines
that you see there,
the leukocyte molecules
undergo changes
that allow them
to get really very sticky,
and you finally get them
to have firm stable adhesion.
05:06
They layer down,
and now, again driven in part
by the chemokines,
they will crawl across.
05:12
The crawl across the endothelium
into the space
where the injury has occurred or
where the infection is happening.
05:19
And then they will follow gradients
that say,
"Over here.
This is where you want to go."
That's where the infection is.
05:26
And they will use
the extracellular matrix to crawl.
05:31
And they will get to the spot
where they then are going to
elaborate their mediators,
and they will eat,
they will phagocytize.
05:37
So this process, multiple stages,
a lot of important molecules
that are involved,
and there are therapeutic
opportunities throughout this.
05:45
So we'll come back
to each of these individual stages.
About the Lecture
The lecture Cellular Response: Introduction by Richard Mitchell, MD, PhD is from the course Acute and Chronic Inflammation.
Included Quiz Questions
Which of the following mediators is produced by neutrophils during acute inflammation?
- Reactive oxygen species
- Histamine
- Complement component C3b
- Immunoglobulins
- von Willebrand factor
What is the correct order of the stages of neutrophil migration during acute inflammation?
- Stasis, rolling, integrin activation, stable adhesion, migration through the endothelium
- Rolling, integrin activation, stable adhesion, stasis, migration through the endothelium
- Vasoconstriction, rolling, integrin activation, stable adhesion, migration through the endothelium
- Integrin activation, rolling, stable adhesion, migration through the endothelium
- Stable adhesion, rolling, integrin activation, migration through the endothelium
Which of the following changes takes place in the capillary bed during inflammation?
- Arteriolar dilation
- Decreased vascular permeability
- Venular constriction
- Contraction of the capillary bed
- Increased intravascular oncotic pressure
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |